Learning About Long QT Syndrome (LQTS) in Children
What is long QT syndrome (LQTS)?
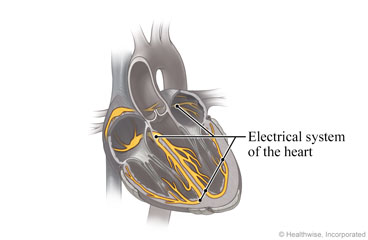
Long QT syndrome (LQTS) is a rare problem that affects the heart's electrical system. It may cause the heart
to beat in a fast and abnormal way. This can cause fainting, seizures, or abnormal heartbeats that can become
life-threatening. If the heart stops pumping blood, sudden death can happen.
What causes it?
A person can be born with LQTS. The gene for it can be passed down in families. So if one family member has
it, other members of the family are more likely to have it too.
Or something else can cause it. It could be a reaction to a medicine. It may be caused by a condition that
causes vomiting or diarrhea. A severe lack of nutrition also can cause it. These problems can cause a mineral
imbalance in the blood that can affect how the heart works.
What are the symptoms?
Some people don't have symptoms. But in those who do, symptoms include fainting, seizures, and feeling dizzy
or lightheaded. Heart palpitations also can occur. LQTS can also cause sudden cardiac arrest. This means that
the heart suddenly stops beating. In some people, symptoms may be triggered by exercise, stress, or being
startled.
How is it diagnosed?
The doctor will do a physical exam. The doctor will also ask questions about your child's symptoms and past
health. And you'll be asked about your family history.
Most children are diagnosed using an electrocardiogram (EKG). It shows the heart's electrical activity as
line tracings on paper. Children with LQTS have a certain pattern to their heartbeat. The doctor can see the
pattern on the tracing.
The doctor may want to do other tests too, such as a test to measure your child's heartbeat during exercise.
Or the doctor may ask your child to wear a small device at home. This device measures your child's heartbeat
during regular activity outside of the doctor's office.
A test may also be done to see if your child carries the gene that causes LQTS. Your child's close relatives
may also get tests. Not everyone with the gene will have symptoms.
How is it treated?
Learning that your child has a heart problem can be scary. But there are treatments that can help your child.
The goals of treatment are to prevent life-threatening heart rhythms and to control symptoms. Treatment
depends on the symptoms and what type of LQTS your child has.
For instance, if your child got LQTS later in life, treatments include stopping any medicines that can cause
the problem and fixing any mineral imbalances your child has. If that doesn't work, or if your child was born
with LQTS, treatments may include:
-
Medicines called beta-blockers. They help control your child's heartbeat.
-
A device called a pacemaker. It's implanted under the skin of your child's chest. It helps control the
heartbeat.
-
A device called an implantable cardioverter-defibrillator. It's implanted in your child's chest. It uses a
shock to stop a dangerous heart rhythm.
-
Surgery to remove nerves that make abnormal heartbeats more likely.
How can you care for your child?
There are things you can do to help prevent a dangerous heart rhythm from LQTS.
-
Tell all of your child's doctors and your pharmacist about your child's condition.
They can help you
avoid medicines that can start a fast or abnormal heartbeat.
-
Ask the doctor for a list of over-the-counter medicines your child shouldn't take.
Some common
medicines, such as certain antacids and antihistamines, can trigger abnormal heartbeats in children with
LQTS.
-
Talk to the doctor about whether lifestyle changes can help.
Some children with LQTS may need to avoid
loud noises, such as alarm clocks and loud ringtones.
-
Ask the doctor about safe levels of activity.
Most people with LQTS should avoid intense physical
activity. Talk to the doctor about what type of activity and exercise is safe for your child.
Follow-up care is a key part of your child's treatment and safety. Be sure to make and go to all
appointments, and call your doctor if your child is having problems. It's also a good idea to know your
child's test results and keep a list of the medicines your child takes.
Current as of: June 24, 2023
Content Version: 14.0
Care instructions adapted under license by your
healthcare professional. If you have questions about a medical condition or this instruction, always ask
your healthcare professional. Healthwise, Incorporated disclaims any warranty or liability for your use of
this information.